What happens after cancer treatment ends?
When we hear the word “cancer” in Malaysia, the conversation usually revolves around breast, lung, or colorectal cancers. But there is a silent battle happening right under our noses—literally. Head and neck cancers are a significant health burden in our country, yet they remain highly misunderstood.
From the pak cik who has been smoking for 40 years to the young professional exposed to the Human Papillomavirus (HPV), head and neck cancers do not discriminate. In fact, Nasopharyngeal Carcinoma (NPC)—a type of head and neck cancer—is one of the top five most common cancers in Malaysia, exceptionally prevalent among the Malaysian Chinese and indigenous communities in Sarawak like the Bidayuh.
If you or a loved one has recently been diagnosed, or if you are currently navigating life after treatment, your mind is likely racing with questions. Do I need surgery? Will I ever be able to eat my favorite nasi lemak again? What happens if the cancer comes back? Do I need to see a doctor for the rest of my life?
In this comprehensive guide, we are going deep into everything Malaysians need to know about head and neck cancers. We will explore treatment options, the realities of cancer recurrence, how to screen for it, and why lifelong follow-up isn’t just a recommendation—it is your lifeline.
Understanding Head and Neck Cancers
Before we dive into treatments and recurrence, we need to understand what we are dealing with. “Head and neck cancer” is a broad term used to describe a range of tumors that develop in or around the throat, larynx (voice box), nose, sinuses, and mouth.
Common Types in Malaysia
- Nasopharyngeal Carcinoma (NPC): Cancer of the upper part of the throat behind the nose. Highly prevalent in Malaysia, often linked to the Epstein-Barr Virus (EBV), genetic predisposition, and diets high in salt-cured foods (like salted fish).
- Oral Cavity Cancer: Cancer of the mouth, tongue, gums, and lips. Historically common among older Malaysians who practice betel quid (sireh) chewing, but increasingly linked to smoking, vaping, and heavy alcohol consumption.
- Laryngeal Cancer: Cancer of the voice box. Almost exclusively linked to tobacco use.
- Oropharyngeal Cancer: Cancer of the middle part of the throat, including the tonsils. Globally and locally, there is a rising trend of these cancers linked to HPV infections.
Consult us for more information
Treatment Options – Surgery vs. No Surgery

One of the most terrifying moments for a patient is the consultation with the oncologist or ENT (Ear, Nose, and Throat) surgeon to discuss the treatment plan.
Many Malaysians fear surgery, often seeking “alternative” traditional treatments out of fear of losing their voice or having facial disfigurement. However, modern medicine at facilities like Hospital Kuala Lumpur (HKL), Institut Kanser Negara (IKN), and various private medical centers has advanced tremendously.
The choice between surgery and non-surgical treatments depends entirely on the tumor’s location, stage, and the patient’s overall health.
1. When is Surgery the Best Option?
Surgery is often the first line of defense for tumors in the oral cavity (mouth) and early-stage cancers of the larynx. The goal is straightforward: physically remove the tumor and a margin of healthy tissue around it to ensure no cancer cells are left behind.
- Minimally Invasive Surgery: For early-stage tumors, surgeons can use lasers or robotic surgery (Transoral Robotic Surgery – TORS) to remove the cancer through the mouth without any external cuts.
- Neck Dissection: If cancer has spread to the lymph nodes in the neck, a surgeon will perform a neck dissection to remove these nodes.
- Reconstructive Surgery: A major fear is cosmetic damage. Today, Malaysian surgeons are highly skilled in reconstructive surgery, using tissue, skin, or bone from other parts of the body (like the forearm or leg) to rebuild the jaw, tongue, or throat, ensuring patients can still swallow, speak, and look like themselves.
2. When is Surgery Avoided? (Non-Surgical Treatments)
Sometimes, surgery is not the primary option. For example, Nasopharyngeal Carcinoma (NPC) is highly sensitive to radiation and is located in a very difficult area to reach surgically without damaging the brain or eyes. Therefore, surgery is rarely the first choice for NPC.
- Radiotherapy (Radiation): Uses high-energy rays to kill cancer cells. Advanced techniques like IMRT (Intensity-Modulated Radiation Therapy) are widely used in Malaysia to target the tumor precisely while sparing healthy tissues like the salivary glands.
- Chemotherapy: Often combined with radiation (chemoradiation) for advanced stages to shrink tumors and kill cancer cells that may have spread.
- Targeted Therapy: Drugs that specifically target cancer’s specific genes, proteins, or the tissue environment that contributes to cancer growth.
- Immunotherapy: A groundbreaking treatment available in Malaysia that stimulates the patient’s own immune system to recognize and destroy cancer cells. This is increasingly used for recurrent or metastatic head and neck cancers.
The Verdict: There is no “one size fits all.” A multidisciplinary team (MDT) of surgeons, oncologists, dietitians, and speech therapists will sit together to tailor the exact protocol for you.
Do These Cancers Need Lifelong Follow-Up?
The short answer is: Yes, absolutely.
When a doctor tells you that you are “in remission” or “cancer-free,” it is a day of massive celebration. Ring the bell, belanja your family to a nice meal, and breathe a sigh of relief. However, remission does not mean the journey is over.
Head and neck cancers are notorious for their ability to return. Because of this, the concept of “lifelong follow-up” is a non-negotiable part of survivorship.
The Critical 5-Year Window
The highest risk of the cancer coming back (recurrence) is within the first two to three years after completing treatment. During this time, you will see your doctors very frequently:
- Year 1: Every 1 to 3 months.
- Year 2: Every 2 to 6 months.
- Years 3 to 5: Every 4 to 8 months.
- Beyond Year 5: Annually.
Why Keep Going After 5 Years?
Even if you hit the golden 5-year mark, lifelong follow-up is necessary for three major reasons:
- Late Recurrence: While rare, some tumors can return a decade later.
- Second Primary Cancers: Head and neck cancer survivors have a significantly higher risk of developing a brand new, different cancer in the head, neck, esophagus, or lungs.
- Managing Late Side Effects of Treatment: Radiation to the neck can cause long-term issues like hypothyroidism (underactive thyroid), chronic dry mouth, dental decay, or difficulties swallowing (dysphagia) years down the line. Regular check-ups help manage these to keep your quality of life high.
External Link: Learn more about post-treatment survivorship from the National Cancer Society Malaysia (NCSM)
Why Do These Cancers Come Back?
Hearing that the cancer has returned is devastating. Many patients ask, “But the doctor cut it all out! I did 35 rounds of radiation! Why did it come back?”
Understanding the “why” involves looking at the microscopic biology of cancer.
1. Microscopic Residual Disease
Even the most brilliant surgeon in Kuala Lumpur cannot see a single microscopic cancer cell with the naked eye. If even a few malignant cells remain in the margins of the tissue removed, or if they survived the radiation, they can slowly multiply over months or years until they form a new tumor.
2. Field Cancerization
This is a crucial concept, especially for Malaysians with a history of heavy smoking, vaping, chewing betel nut, or drinking alcohol. When you expose your mouth and throat to carcinogens for decades, the entire lining of your upper airway is damaged at a cellular level.
Even if the primary tumor is successfully treated, the surrounding “normal-looking” tissue is already genetically mutated. Over time, these pre-cancerous fields can spawn a completely new tumor.
3. Cancer Stem Cells
Tumors are not uniform. Within a tumor, there are “cancer stem cells” that are highly resilient. They act like seeds. While chemotherapy and radiation might kill 99% of the rapidly dividing cancer cells (the “weeds”), the deep-rooted “seeds” might go dormant, survive the treatment, and sprout again when the conditions are right.
4. Treatment Resistance
Sometimes, the cancer cells simply adapt. They mutate to become resistant to the chemotherapy drugs or the radiation therapy that once worked so well against them.
How to Know if It Comes Back? (Signs and Symptoms)
Vigilance is your best friend. As a survivor, you know your body better than anyone else. If you notice any of the following symptoms lasting for more than two weeks, you should contact your medical team immediately. Do not wait for your next scheduled appointment.
Look Out For:
- A New Lump or Swelling: Especially in the neck. Neck lumps are often the first sign that cancer has spread to the lymph nodes.
- A Sore That Won’t Heal: Any ulcer or patch (red or white) in the mouth or throat that bleeds easily and doesn’t resolve.
- Pain: Persistent pain in the mouth, throat, or—very commonly—referred pain in the ear. (Because the nerves in the throat share pathways with the ear, a tumor in the throat often feels like an earache).
- Changes in Voice: Persistent hoarseness or a raspy voice.
- Difficulty Swallowing (Dysphagia): Feeling like food is stuck in your throat, or pain when swallowing.
- Unexplained Weight Loss: Dropping weight without trying is always a red flag in oncology.
- Nasal Symptoms: Chronic blocked nose on one side, frequent nosebleeds, or blood in your phlegm (especially for NPC survivors).
Internal Link Placeholder: [Download our free printable symptom tracker checklist for head and neck cancer survivors]
How to Screen and Monitor for Recurrence

So, how do doctors actually check if the cancer has returned? You can’t just rely on symptoms, because the goal of follow-up is to catch a recurrence before symptoms even appear.
In Malaysia, your follow-up routine at a government hospital or private specialist clinic will involve a combination of the following:
1. The Physical Examination
Your ENT surgeon or oncologist will perform a thorough physical exam. They will feel your neck for enlarged lymph nodes, check the inside of your mouth, and examine your throat.
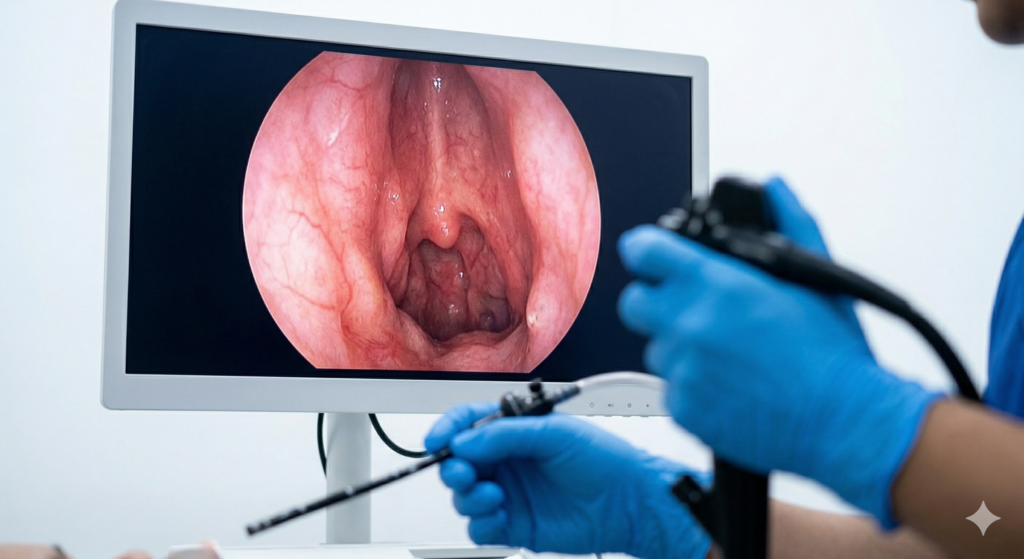
2. Endoscopy (Nasendoscopy)
This is a staple of head and neck follow-ups. The doctor will insert a thin, flexible tube with a camera and a light at the end (an endoscope) into your nose to look down at your nasal cavity, throat, and vocal cords. It sounds uncomfortable, but local anesthetic spray is used, and it takes less than two minutes. It gives the doctor a high-definition view of areas that cannot be seen from the outside.
3. Imaging Scans
You won’t need scans at every single visit, but they are crucial tools.
- CT Scans / MRI: Used to look at the deep tissues of the head and neck to see if any masses are growing beneath the surface. MRIs are particularly excellent for soft tissue evaluation.
- PET-CT Scans: The ultimate detective tool. A PET scan uses a safe amount of radioactive sugar injected into your blood. Because cancer cells consume energy much faster than normal cells, they “light up” on the scan. This helps doctors distinguish between a returning cancer and normal post-radiation scar tissue.
4. Blood Tests
While there isn’t a definitive standard blood test for all head and neck cancers, specific markers are used. For Nasopharyngeal Carcinoma (NPC), doctors often track the EBV DNA blood test. A rising level of Epstein-Barr Virus DNA in the blood can be an early warning sign that the cancer is returning, long before a scan shows a tumor.
5. Biopsy
If your doctor sees something suspicious during an endoscopy or on a scan, they will take a biopsy (a small tissue sample) to be examined under a microscope. A biopsy is the only 100% definitive way to confirm a recurrence.
External Link: Ministry of Health Malaysia (KKM) Guidelines on Cancer Screening
Financial and Emotional Support in Malaysia
Dealing with cancer recurrence or the anxiety of follow-ups (often called “scan-xiety”) is incredibly taxing. It is vital to remember that you are not walking this path alone.
Financial Aid
Cancer treatments, especially targeted therapies and immunotherapies, can be financially draining. Malaysians have several avenues for support:
- Government Hospitals: Treatment at KKM facilities is highly subsidized and offers world-class care.
- MySalam & Peka B40: Government initiatives that provide financial payouts and subsidized screenings for low-income brackets.
- SOCSO (Perkeso): If you are a contributor, you may be eligible for invalidity pensions or assistance with medical rehabilitation equipment.
- MAKNA (Majlis Kanser Nasional): Provides bursary assistance to poor patients for treatment, travel, and nutritional milk formulas.
Emotional Support
Mental health is just as important as physical health. Joining a support group where you can speak to other survivors in Malaysia who understand exactly what you are going through is life-changing.
Conclusion: Taking Control of Your Journey
Head and neck cancers are formidable opponents, and the fear of recurrence is a heavy burden to carry. But knowledge is power. By understanding why lifelong follow-ups are necessary, recognizing the early warning signs, and staying diligent with your medical team, you dramatically tip the scales in your favor.
Whether your treatment involved a complex surgery or a rigorous round of chemoradiation, your body has fought a massive war. Respect that battle by attending your follow-up appointments, living a healthier lifestyle (put down that cigarette or vape!), and giving yourself grace.
Have you or a loved one navigated head and neck cancer? What was your experience with follow-up care in Malaysia? Share your story in the comments below—your journey could be the hope someone else desperately needs to read today.
Disclaimer: The information provided in this article is for educational purposes only and should not replace professional medical advice. Always consult your oncologist or ENT specialist regarding your specific health condition and treatment plan.
Discover more from The ENT Doctor
Subscribe to get the latest posts sent to your email.


No responses yet