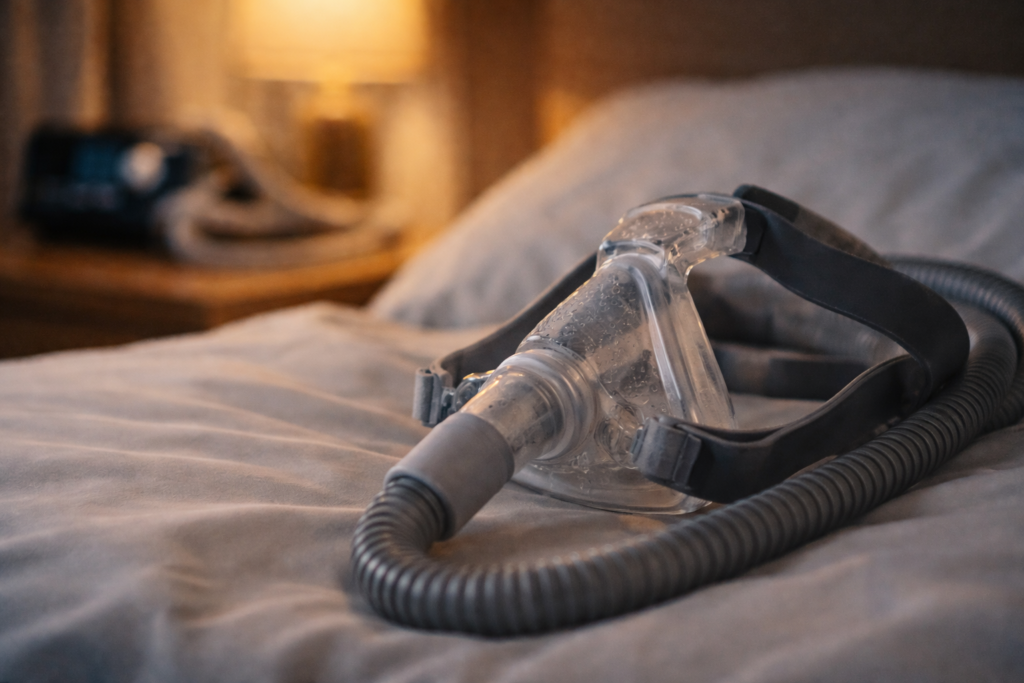
If you have obstructive sleep apnea (OSA), CPAP is often the first treatment offered. It works well when you can use it consistently.
But some people simply cannot tolerate CPAP. The mask leaks. The pressure feels suffocating. The nose is blocked. The mouth dries out. Or the device just makes sleep worse.
If that is you, you are not “failing.” You are looking for the next best plan.
This article explains the main surgical options for OSA, who they suit, and what the usual work-up looks like.
Important note: Surgery is not “one size fits all.” The best choice depends on where your airway collapses, your sleep study severity, and your body build and medical risks.
Step 1: Confirm the diagnosis and the pattern
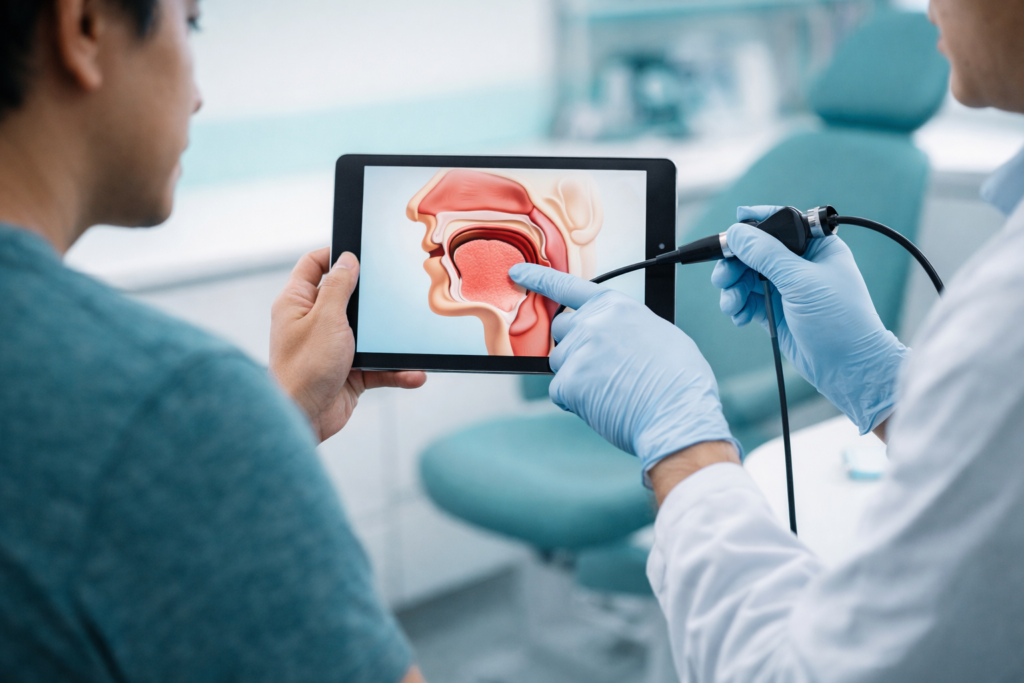
Before discussing surgery, make sure you have:
- A sleep study (home test or PSG) with key numbers like AHI, oxygen levels, and sleep time.
- A proper nose and throat examination.
- A discussion of your goals (snoring only vs true OSA control, daytime sleepiness, blood pressure, long-term health).
Many centres also use drug-induced sleep endoscopy (DISE). It is a short procedure where we watch your airway during sedated “sleep” to see the collapse level (palate, tongue, epiglottis, or multi-level). DISE may help match the operation to the blockage.
Step 2: Know what surgery can (and cannot) do
Surgery aims to:
- Widen the airway, or
- Stiffen tissues that collapse, or
- Move skeletal structures forward (jaw surgery), or
- Activate airway muscles (hypoglossal nerve stimulation), or
- Reduce weight-related airway load (bariatric surgery in selected patients)
Some surgeries are adjuncts (help CPAP or oral appliance work better). Some are standalone treatments for selected patients.
If your main problem is a blocked nose
1) Septoplasty and turbinate reduction
If you have significant nasal obstruction (deviated septum, enlarged turbinates, chronic rhinitis), nasal surgery can improve airflow.
What it can do
- Often improves CPAP tolerance (less pressure needed, less mouth breathing).
- May improve snoring and sleep comfort.
What it cannot promise
- Nasal surgery alone usually does not “cure” moderate–severe OSA if collapse is mainly at the palate or tongue.
Best for
- People who cannot use CPAP because they “cannot breathe through the nose.”
If collapse is mainly at the soft palate and tonsil region
2) Tonsillectomy (adults)
Large tonsils can narrow the throat and worsen OSA.
Best for
- Adults with big tonsils and clear narrowing at the oropharynx.
Common benefits
- Can significantly reduce obstruction in the right anatomy.
- Often combined with other palate procedures if needed.
3) Palate surgery (UPPP and modern variants)
You may hear terms like:
- UPPP (uvulopalatopharyngoplasty)
- Expansion sphincter pharyngoplasty
- Other reconstructive palate techniques
The goal is to reduce collapse and widen the retropalatal airway.
Best for
- Palate-dominant collapse (often confirmed on DISE).
Trade-offs
- Recovery pain can be significant.
- Risks include bleeding, voice or swallow changes (uncommon but real), and persistent OSA if other levels still collapse.
If the tongue base is the main obstruction
Tongue base collapse is common in OSA. It is also a common reason why palate-only surgery fails.
4) Tongue base reduction (non-robotic or robotic)
Options vary by surgeon and anatomy. They may include:
- Tongue base reduction techniques (energy-based or tissue reduction)
- Transoral robotic surgery (TORS) for selected tongue base obstruction
Best for
- Documented tongue base obstruction on DISE, especially when symptoms persist after palate work or when tongue base is clearly the main issue.
What to expect
- It is often part of a multi-level plan (palate + tongue, sometimes with epiglottis treatment).
If the epiglottis collapses
5) Epiglottis surgery (selected cases)
Some patients have epiglottic “flop” or collapse during sleep.
Best for
- Epiglottic collapse proven on DISE.
This is a niche area, but it matters because epiglottic collapse can make CPAP uncomfortable in some patients.
If you want an alternative to tissue cutting: nerve stimulation
6) Hypoglossal nerve stimulation (HNS)
This is an implanted device that stimulates the hypoglossal nerve during sleep. It helps move the tongue forward in sync with breathing.
Best for (typical criteria vary by region and funding)
- Adults with moderate to severe OSA
- Unable to use CPAP
- Suitable airway pattern on DISE (commonly, no complete concentric palatal collapse)
- BMI and AHI criteria depend on local rules, payors, and device indications
Professional bodies include HNS among effective options for selected patients.
Pros
- No major throat cutting.
- Many patients like the “on/off” control.
Cons
- Not for everyone.
- It is device-based, with cost considerations and long-term follow-up.
If your jaw structure drives the obstruction
7) Maxillomandibular advancement (MMA)
This is jaw surgery that advances the upper and lower jaw forward, enlarging the airway.
Best for
- Moderate–severe OSA with craniofacial contributors (small jaw, retrusive jaw), or multi-level collapse where MMA is the most definitive option.
Pros
- One of the most effective surgical options for appropriately selected patients.
Cons
- Bigger operation.
- Longer recovery.
- Requires OMFS collaboration and careful planning.
If weight is a major driver
8) Bariatric surgery (for selected patients)
If obesity is a major factor and CPAP cannot be used, weight-loss surgery may be discussed as part of OSA management.
The AASM guideline recommends that in adults with OSA and CPAP intolerance, clinicians should discuss referral:
- to a sleep surgeon if BMI is under 40, and
- to a bariatric surgeon when BMI is 35 or higher (as part of alternative options).
This does not mean bariatric surgery is “the answer” for everyone. It means weight management is a serious part of long-term control for many patients.
What does a “surgical pathway” usually look like?
A practical flow is:
- Confirm OSA on sleep study (AHI, oxygen, symptoms).
- Identify barriers to CPAP (nose blockage, mask fit, pressure, insomnia).
- Examine nose + throat.
- Consider DISE for collapse mapping.
- Decide:
- Nasal-first (if nose is the main barrier),
- Single-level surgery (if one main site),
- Multi-level surgery (common), or
- Device/jaw/weight pathway (HNS, MMA, bariatric).
If you want a patient-friendly overview, the AASM also has a surgical consultation guide that explains what to expect.
“Which surgery is best?”
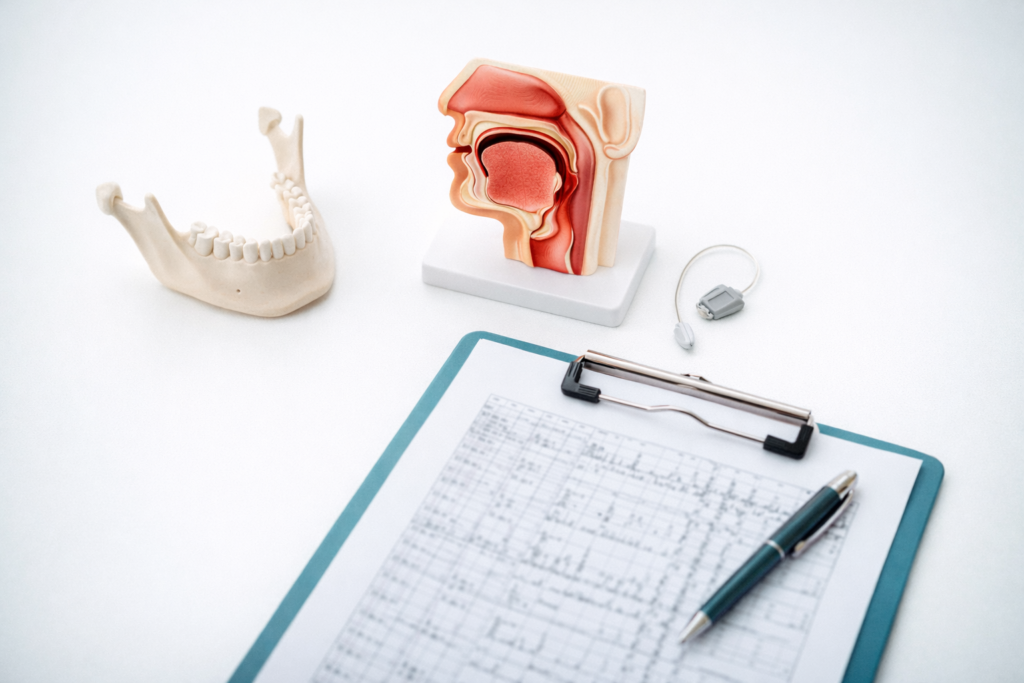
The honest answer: the one that matches your collapse pattern.
Two patients can have the same AHI and need completely different treatments.
This is why a targeted assessment matters. It avoids doing “palate-only” surgery when the real issue is the tongue base. Or doing tongue surgery when the nose is the main reason CPAP failed.
Common questions
Does surgery guarantee I can stop CPAP?
Not always. Some surgeries aim to:
- reduce OSA severity,
- reduce CPAP pressure needs, or
- make CPAP tolerable.
Some patients still need CPAP, but use it far more comfortably.
Is surgery only for severe OSA?
No. Surgery can be considered across severities, depending on symptoms, anatomy, and treatment goals.
What if I’m afraid of pain?
That is valid. Recovery varies by procedure. Ask your surgeon what pain control plan they use and what recovery realistically feels like for that specific operation.
Take-home message
If you cannot use CPAP, you still have options. Good OSA surgery is not about “doing more.” It is about doing the right thing at the right level.
If you want to explore this, start with:
- your sleep study report,
- a focused airway exam, and
- a discussion about DISE and a personalised plan.
Medical disclaimer: This article is general education. It is not personal medical advice. Surgical decisions require in-person assessment, review of your sleep study, and discussion of risks and alternatives.
Internal Links (TheENTDr.com)
- An Overview on Sleep Apnea https://theentdr.com/blog/an-overview-on-sleep-apnea/
- Sleep Studies (PSG / Home Sleep Test) https://theentdr.com/blog/sleep–studies/
- Why Sleep Apnea Comes Back After CPAP, Oral Appliance, or Surgery https://theentdr.com/blog/sleep-apnea-comes-back-after-cpap-oral-appliance-surgery/
- Snoring vs Sleep Apnea (Do Pillows Help?) https://theentdr.com/blog/do-pillows-help-obstructive-sleep-apnea-or-snoring/
- When to Consider Nasal Surgery https://theentdr.com/blog/when-to-consider-nasal-surgery/
- Nose Specialist PJ (services: septoplasty/turbinate/sinus) https://theentdr.com/services/nose-specialist-pj/
- Tonsil & Adenoid Surgery (Before / During / After) https://theentdr.com/blog/before-during-after-tonsil-adenoid-surgery/
- Sleep Specialist PJ (services: DISE + surgical options overview) https://theentdr.com/services/sleep-specialist-pj/
External Links (Credible References)
- AASM Clinical Practice Guideline (Referral for Surgical Consultation in Adults with OSA) https://pmc.ncbi.nlm.nih.gov/articles/PMC8726361/
- AASM Patient Guide (PDF): Referral for OSA Surgical Consultation https://aasm.org/wp-content/uploads/2023/01/Referral-OSA-Surgical-Consultation-Patient-Guide.pdf
- AAO-HNS Position Statement: Treatment of Obstructive Sleep Apnea https://www.entnet.org/resource/position-statement-treatment-of-obstructive-sleep-apnea/
- AAO-HNS Position Statement: Hypoglossal Nerve Stimulation for OSA https://www.entnet.org/resource/position-statement-hypoglossal-nerve-stimulation-for-treatment-of-obstructive-sleep-apnea-osa/
- NICE Evidence Overview: Hypoglossal Nerve Stimulation for OSA https://www.nice.org.uk/guidance/htg455/evidence/overview-final-pdf-4664631853
Discover more from The ENT Doctor
Subscribe to get the latest posts sent to your email.


No responses yet