You are bathing your child, or maybe running your fingers through their hair after a long day, and you feel it — a small lump on the side of the neck. Your heart skips a beat. Questions flood your mind. Is it serious? How long has it been there? Should I go to the hospital right now?
Take a breath. You are not alone, and in most cases, you are not facing something scary.
Swollen lymph nodes in the neck are one of the most common reasons parents bring their children to an ENT clinic. In the vast majority of cases, the cause is something entirely ordinary — a cold, a sore throat, or even a tiny skin scratch the child barely noticed. But knowing when to watch and wait, and when to act, makes all the difference.
This guide is written for you — the parent, the caregiver, the worried grandparent — to help you understand what is happening, what questions to ask, and what to expect every step of the way.
What Are Lymph Nodes, and Why Does My Child Have Them?
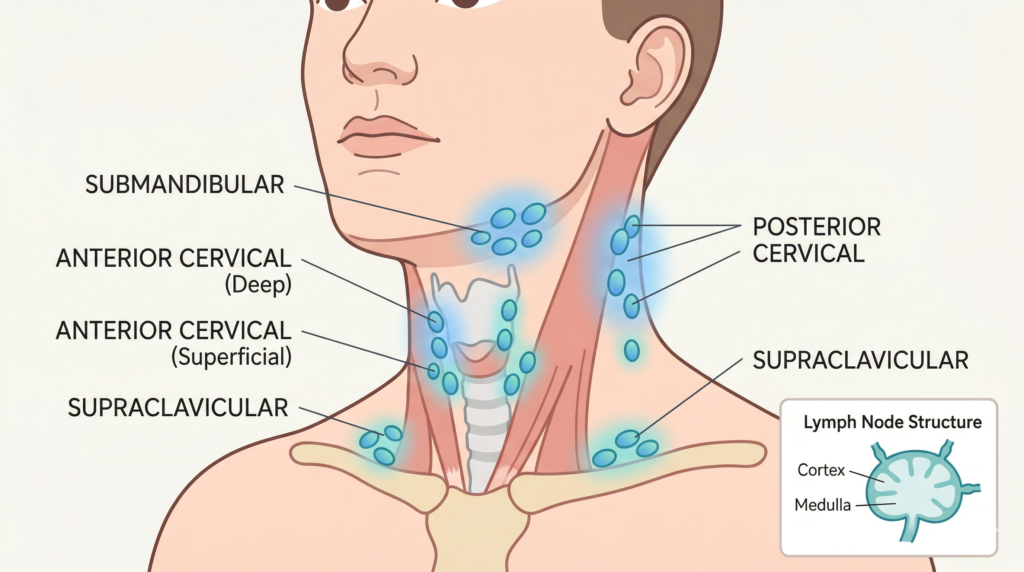
Think of lymph nodes as your body’s security checkpoints. They are small, bean-shaped glands scattered throughout the body — in the neck, armpits, groin, and many places you cannot feel — and they are part of the immune system, your child’s natural defence force against infection and disease.
Inside each lymph node are white blood cells called lymphocytes. When a threat enters the body — a virus, bacteria, or any foreign invader — these white blood cells multiply rapidly to fight it off. That multiplication is what causes the node to swell. In other words, a swollen lymph node is often a sign that your child’s immune system is doing exactly what it should be doing.
Children and adolescents have a lot of lymph nodes in the neck — roughly 300 in that region alone. Because their immune systems are still maturing and constantly encountering new germs (especially once school begins), swollen glands in the neck are extremely common in this age group. In fact, it is perfectly normal for many children to have small, pea-sized nodes that you can feel in the neck at any given time.
The medical term for swollen lymph nodes in the neck is cervical lymphadenopathy (cer-vi-cal lim-fad-en-op-ah-thee). It sounds intimidating, but it simply means enlarged lymph nodes in the cervical — or neck — region.
Why Do Children Get Swollen Lymph Nodes in the Neck?

The short answer: most of the time, because of an infection happening somewhere in the head or neck region.
The lymph nodes in the neck drain fluid from the face, scalp, mouth, throat, ears, and nose. So any infection in those areas can cause the nearby lymph nodes to swell up and do their job.
The Most Common Culprits
Upper respiratory tract infections (URTIs) are the number one cause. The common cold, the flu, and other viral infections are everyday triggers. Your child gets a runny nose and sore throat on Monday, and by Wednesday, you notice a lump in their neck — that is the immune system at work.
Tonsillitis and throat infections are another frequent cause. The tonsils act as the first line of defence against germs that enter through the mouth and nose, so when they are inflamed or infected, the nearby neck lymph nodes almost always swell too. You can read more about this in our post on tonsillitis causes and what to do.
Strep throat, caused by the Streptococcus bacteria, often causes particularly tender, enlarged neck nodes alongside a very sore throat — sometimes without even a runny nose.
Ear infections, especially in younger children, can also trigger neck lymph node swelling. Middle ear infections are common in children and sometimes go hand-in-hand with swollen glands. Our guide on chronic ear infections in children covers this in more detail.
Glandular fever (Infectious Mononucleosis), caused by the Epstein-Barr Virus (EBV), is particularly common in adolescents and teenagers. It often causes significant swelling of lymph nodes on both sides of the neck, along with extreme fatigue, a severe sore throat, and sometimes a fever that lingers for weeks. It is sometimes called the “kissing disease” because it spreads through saliva — a useful piece of trivia for the parents of teenagers.
Skin infections and scalp conditions — a small pimple, an infected insect bite on the scalp, or a skin rash can cause nearby lymph nodes to swell in response.
Dental infections — tooth abscesses or gum infections around the jaw can sometimes cause lumps that feel like they are in the neck.
Less Common Causes
A small number of children with swollen neck nodes have causes that need closer attention:
- Bacterial lymphadenitis — when the lymph node itself becomes infected, often by Staphylococcus or Streptococcus bacteria. The node becomes larger, redder, warmer, and more painful than usual, and may eventually fill with pus.
- Tuberculosis (TB) — though less common in many settings, TB affecting the neck lymph nodes (called scrofula) does occur, especially in children with exposure history. We have a dedicated post on TB and ENT symptoms in Malaysia if this is a concern.
- Cat scratch disease — caused by bacteria from a cat scratch or bite, which can cause persistent swelling of nearby nodes.
- Non-Hodgkin’s lymphoma or Hodgkin’s lymphoma — cancers of the lymphatic system. These are rare, but they are the reason we take persistent or unusual lymph node swelling seriously. The good news is that when caught early, these conditions are very treatable.
- Other tumours — very rarely, a lump in the neck can represent another type of cancer or a metastasis from a tumour elsewhere.
It cannot be stressed enough: the vast majority of children — well over 90% — with swollen neck lymph nodes have a completely benign, self-limiting cause. But the role of the ENT and paediatric specialist is to identify the rare child who needs more attention.
What Does It Look Like? Knowing What to Feel For
When you run your fingers along the side of your child’s neck, a normal or reactive (reactive = responding to an infection) lymph node typically feels:
- Soft or slightly firm, not rock hard
- Smooth and round, like a small pea or grape
- Moveable — you can gently slide it under the skin
- Slightly tender when pressed, but not excruciatingly painful
- Less than 1–2 cm in size (about the width of your thumbnail)
Reactive nodes on both sides of the neck (bilateral) are particularly reassuring, as they suggest a general infection rather than something localised and potentially more serious.
When Should You Be Worried? The Red Flags
While most cases are harmless, certain signs should prompt you to seek medical attention sooner rather than later. If you notice any of the following, do not wait — book an appointment with an ENT or your paediatrician:
Size matters. A lymph node that is larger than 2 cm (roughly the size of a 50 sen coin) warrants a professional evaluation, even without other symptoms.
It keeps growing. If the lump is getting bigger over several weeks instead of shrinking, that is a signal to investigate further.
It has been there too long. Nodes from a typical infection should start shrinking within 2–4 weeks of the infection clearing. Swelling that persists beyond 6 weeks needs a proper assessment.
It feels hard and does not move. A lymph node that feels rubbery or hard, and which does not shift when you press it (described as “fixed”), is a feature that specialists take very seriously.
It is above the collarbone. A swollen lymph node in the supraclavicular region (just above the collarbone) is considered a red flag in any age group, regardless of size.
There is accompanying fever, night sweats, or unexplained weight loss. This combination — sometimes called “B symptoms” in the medical world — alongside enlarged lymph nodes raises the concern for lymphoma and requires urgent evaluation.
The skin over the node is red, warm, or there is a discharge. This could indicate a bacterial infection or abscess that needs treatment, sometimes surgical drainage.
Your child has difficulty swallowing or breathing. This is an emergency. Seek care immediately.
The lump appeared after a neck injury or blow to the head. Less concerning in isolation, but worth mentioning to a doctor.
If you are unsure, the golden rule is simple: if it worries you, get it checked. ENT specialists see neck lumps every day, and a review — even if everything turns out to be fine — gives you peace of mind and catches the rare serious case early.
When Should You See an ENT Specialist?
Your GP or paediatrician is a great first point of contact for most neck lumps in children. They will often monitor a swollen node during and after an infection before referring you onward.
However, there are situations where going directly to an ENT specialist makes sense:
- The lump has been present for more than 4–6 weeks
- The lymph node is growing rapidly
- The node is larger than 2 cm
- There are multiple swollen nodes at different levels of the neck
- Your child has had repeated neck infections or tonsil infections
- There is a concern about a deeper infection such as a neck abscess — a condition we have written about in our post on deep neck infections
- Your GP is uncertain and wants a specialist’s opinion
At The ENT Doctor in Petaling Jaya, our paediatric ENT services are designed specifically around the needs of children and their families. We understand that children are not just small adults — they need a different approach, a calmer environment, and a doctor who explains things clearly to both the child and the parents.
What Will the ENT Doctor Do?
Walking into a specialist clinic can feel nerve-wracking, especially when your child is the patient. Here is exactly what you can expect during a consultation for a neck lump.
Step 1: History Taking
The doctor will ask you a series of questions. Do not be put off by how many there are — each one helps build a picture. Expect questions like:
- How long have you noticed the lump?
- Has your child been sick recently — a cold, sore throat, ear infection?
- Has the lump grown, stayed the same, or gotten smaller?
- Does your child have a fever, night sweats, or unexplained weight loss?
- Has your child been in contact with animals, especially cats?
- Has your child been abroad recently, or been exposed to anyone with TB?
- Any family history of cancer?
Step 2: Physical Examination
The doctor will gently examine the neck, feeling each lymph node group carefully. They will assess the size, firmness, tenderness, and mobility of the nodes. They will also examine the throat, tonsils, ears, nose, and mouth — because finding an infection source nearby often explains the swollen node entirely.
Step 3: Investigations (If Needed)

Not every child with a swollen lymph node needs blood tests or scans. But if the history or examination raises any concern, the doctor may order:
Blood tests, including a full blood count (to check for infection or abnormal blood cells), inflammatory markers (ESR, CRP), and sometimes specific tests for EBV, CMV, or TB.
Ultrasound of the neck — this is a very child-friendly investigation. No radiation, no needles, just a gel and a probe on the neck. It gives the doctor excellent information about the size, shape, and internal characteristics of a lymph node. Certain ultrasound features can be very reassuring; others prompt further investigation.
CT scan or MRI — reserved for more complex cases, especially when there is concern about a deep infection, a collection of pus, or a suspicious mass.
Fine needle aspiration (FNA) — a thin needle is used to take a small sample of cells from the node for examination under a microscope. It sounds scarier than it is. In cooperative older children and adolescents, it can often be done in the clinic with local anaesthetic cream applied beforehand.
Excisional biopsy — if there is a strong clinical reason to suspect lymphoma or another serious condition, the surgeon may recommend removing the lymph node entirely for detailed laboratory analysis. This is done under general anaesthesia and is the most reliable way to make a definitive diagnosis.
What Can Be Done? Treatment Options Explained
Treatment depends entirely on the cause. Here is how the most common scenarios play out:
Viral Infections — Watch and Wait
If the swollen nodes are clearly due to a viral cold or similar infection, no specific treatment is needed for the lymph nodes themselves. They will settle on their own, typically within 2–6 weeks of the illness resolving. The doctor may recommend:
- Adequate rest and fluids for your child
- Paracetamol or ibuprofen for pain or fever
- A review appointment in 4–6 weeks to ensure the nodes are shrinking
This “watchful waiting” approach is entirely appropriate and evidence-based. Prescribing antibiotics for a viral illness does not help and carries its own risks.
Bacterial Infections — Antibiotics
If bacteria are identified as the cause (for example, strep throat, a skin infection, or a dental abscess), a course of antibiotics targeted at the specific bacteria involved will be prescribed. Most children respond well within a few days, and the lymph nodes gradually shrink over the following weeks.
Bacterial Lymphadenitis with Abscess — Drainage
If the lymph node itself has become infected and filled with pus (an abscess), it may need to be drained surgically. This is done under general anaesthesia and is very effective. After drainage, antibiotics are continued to clear the infection completely.
Glandular Fever — Rest and Recovery
There is no specific antiviral treatment for infectious mononucleosis. The mainstay is rest, hydration, and time. Contact sports must be avoided for at least 4 weeks due to the risk of splenic rupture — the spleen enlarges during EBV infection, and a blow to the abdomen can be dangerous. Most adolescents recover fully, though fatigue may linger for several weeks.
TB Lymphadenitis — Anti-TB Medication
TB affecting the neck nodes requires a course of anti-tuberculosis medication, typically for 6 months. The ENT specialist works closely with an infectious disease or respiratory physician in these cases.
Lymphoma or Other Cancers — Oncology Team
If the investigations confirm a diagnosis of lymphoma or another malignancy, care is transferred to a paediatric oncology team. Modern treatments for childhood lymphoma — including chemotherapy and sometimes radiotherapy — have excellent outcomes, especially when caught early. The ENT surgeon often plays a key role in obtaining the tissue diagnosis that leads to treatment.
What Should You Expect? The Timeline
One of the most common questions parents ask is: “How long will this take to go away?”
Here is a realistic timeline for the most common scenario — a reactive lymph node from a viral infection:
| Timepoint | What Typically Happens |
|---|---|
| Week 1–2 | Node may continue to enlarge while the infection is active |
| Week 3–4 | Infection clears; node begins to soften and shrink |
| Week 6–8 | Node significantly smaller, though may remain palpable |
| 3–6 months | Most nodes return to normal or near-normal size |
It is completely normal for a lymph node to remain slightly enlarged for weeks to months after an infection. This does not mean the infection is still active. The node is simply returning slowly to baseline.
If a node is not following this trajectory — if it is growing instead of shrinking, or if it remains the same size after 6 weeks — that is when the doctor will want to reassess.
Frequently Asked Questions
My child’s lymph node is hard and I am very scared. Does that mean cancer?
Not necessarily. While hardness is a feature that specialists note, many benign conditions can cause firmer nodes. Context matters enormously — the size, duration, other symptoms, and your child’s overall health all contribute to the assessment. Please do not catastrophise before seeing a doctor. Get it examined and take it from there.
Is it okay to massage or press on the lymph node?
Light touching is fine and will not cause harm. Vigorous rubbing will not make it go away faster and might make it sore. The urge to check it every hour is very human, but try to resist — it will not change anything and will increase your anxiety.
My toddler has two swollen glands — could they both be serious?
Bilateral (both sides) swelling in young children is almost always due to a viral infection, especially if your toddler has recently had a runny nose or cold. It is one of the most reassuring patterns a doctor can see.
Can swollen lymph nodes in the neck cause difficulty breathing?
In most cases, no. However, very large or rapidly growing nodes, or a collection of nodes forming a mass, could theoretically cause pressure symptoms. This is very rare, but if your child is struggling to breathe or swallow, seek emergency care immediately.
Should I avoid any foods or activities if my child has swollen neck glands?
No specific dietary restrictions are needed. Keep your child hydrated and rested during any active infection. If glandular fever is diagnosed, contact sports must be avoided as noted above.
At what age do lymph nodes stop being a concern?
Swollen lymph nodes can occur at any age. They are simply more commonly seen in children because children encounter so many new germs as their immune systems develop. The approach to evaluation does shift somewhat in adults, where the threshold for concern can be a little lower.
A Word From The ENT Doctor
Swollen lymph nodes in a child’s neck are one of the things that can send a parent into a spiral of worry at 2am. We see this every week at our clinic. And almost every week, we get to give families the reassurance that what their child has is completely normal and will settle on its own.
But we also occasionally find the rare child who needs prompt investigation, and finding that child early makes a real difference in their outcome. That is why we take every neck lump seriously — not because every lump is dangerous, but because every family deserves a proper answer.
If you are concerned about a lump in your child’s or teenager’s neck, do not leave it to chance. Book a consultation with our paediatric ENT team or our head and neck specialist in Petaling Jaya. A thorough assessment is the fastest way to peace of mind.
You may also find these related reads helpful before your visit:
- Neck Swelling: What to Do and What to Expect
- Paediatric ENT Guide: Caring for Your Child’s Ear, Nose & Throat Health
- Before, During and After Tonsil & Adenoid Surgery
- Noisy Sleep in Children: When Should You Be Concerned
External Links
- Cleveland Clinic — Cervical Lymphadenopathy
https://my.clevelandclinic.org/health/symptoms/25248-cervical-lymphadenopathy - Stanford Children’s Health — Lymphadenopathy in Children
https://www.stanfordchildrens.org/en/topic/default?id=lymphadenopathy-in-children-90-P02044 - Nationwide Children’s Hospital — Lymphadenopathy in Children
https://www.nationwidechildrens.org/conditions/health-library/lymphadenopathy-in-children - Mayo Clinic — Swollen Lymph Nodes
https://www.mayoclinic.org/diseases-conditions/swollen-lymph-nodes/symptoms-causes/syc-20353902 - PMC / NCBI — An Approach to Cervical Lymphadenopathy in Children (Peer-reviewed)
https://pmc.ncbi.nlm.nih.gov/articles/PMC8040913/ - PMC / NCBI — Etiologies of Pediatric Cervical Lymphadenopathy: A Systematic Review (Peer-reviewed)
https://pmc.ncbi.nlm.nih.gov/articles/PMC6661788/
Ready to get answers? Contact us here or visit us at our clinic in Petaling Jaya.
Discover more from The ENT Doctor
Subscribe to get the latest posts sent to your email.


No responses yet